As a pharmacist, I’ve dispensed thousands of diabetes medications. But the most important prescription I ever gave? Understanding how stress affects blood sugar faster than a slice of cake.
The 3 AM Mystery That Changes Everything

Nomsa stared at her glucose monitor in disbelief: 13.7 mmol/L at 3 AM.
She’d done everything right. Perfect meal plan. Metformin on schedule. Even that 30-minute post-dinner walk. Yet here she was, watching numbers that made no sense.
“I must be failing again,” she whispered, shame flooding through her.
What Nomsa didn’t know? That shame response had just triggered a hormone cascade that would keep her blood sugar elevated for the next 6-8 hours. The culprit wasn’t her diet or medication compliance.
It was cortisol – and understanding how stress affects blood sugar is crucial knowledge most people never learn about.
This shame-cortisol-glucose connection drives more than just nighttime spikes. Learn why you crave sugar at night when stress hormones disrupt your overnight blood sugar patterns.
Does Stress Really Affect Blood Sugar? The Science Says Yes

Here’s the short answer: Yes, stress absolutely affects blood sugar, and the impact is immediate and measurable.
Many people wonder “does stress affect blood sugar?” and the answer is definitively yes. However, understanding how stress affects blood sugar requires knowing about cortisol – the body’s primary stress hormone.
When you’re stressed (whether from traffic, work pressure, or self-judgment), the body can’t tell the difference between real danger and emotional pressure. The response is identical: cortisol floods the system, instantly converting stored energy into glucose.
This made sense when our ancestors faced charging animals. But today? The body treats a moment of shame about blood sugar the same way it would treat a life-or-death situation.
How Stress Affects Blood Sugar: The 4-Phase Process
Understanding exactly how stress affects your blood sugar happens in four distinct phases:
Phase 1: The Stress Signal (0-30 seconds)
Initially, the brain detects stress and sends an urgent message to adrenal glands: “Release cortisol. Now.” This happens whether the stress is physical danger or emotional distress.
Phase 2: The Glucose Flood (30 seconds – 2 minutes)
Next, cortisol hits the liver like a biochemical crowbar, forcing it to break down stored glycogen into glucose. Furthermore, research confirms that cortisol directly increases glucose production – the body literally manufactures glucose from stored proteins and fats¹. As a result, blood sugar spikes, regardless of what you’ve eaten.
Phase 3: The Insulin Block (2-30 minutes)
Subsequently, here’s where stress affects blood sugar most dangerously. Cortisol doesn’t just raise glucose – it actively prevents insulin from working properly. Moreover, studies show chronic cortisol elevation creates insulin resistance by interfering with insulin signaling pathways². Essentially, it’s like having a key that won’t turn in the lock.
Phase 4: The Craving Storm (30 minutes – 6 hours)
Finally, the brain senses high glucose but blocked insulin signals, so it panics. Consequently, this triggers intense cravings for quick energy – usually sugar or refined carbs. Therefore, this explains exactly how stress affects blood sugar over extended periods.
These stress-driven cravings follow predictable patterns throughout your day. Learn more about cortisol sugar cravings and why your inner critic makes you hungry during high-stress moments.
Why Your Doctor Isn’t Talking About Stress and Blood Sugar
Most diabetes education focuses on the “Big Three”: medication, diet, and exercise. Very crucial. All necessary.
But incomplete.
After 15 years in South African pharmacies, I’ve watched countless patients follow protocols perfectly yet still struggle with unexplained glucose spikes. The missing piece? Understanding how stress affects blood sugar – a connection that no one discusses.
Consider this: A single moment of self-criticism can raise blood sugar as much as eating a koeksister. Yet we obsess over carb counting while ignoring stress management.
The Pharmacy Counter Breakthrough

My understanding of how stress affects blood sugar changed during a busy Thursday at a Cape Town pharmacy. Mrs. Patel approached my counter with tears in her eyes.
“My numbers are perfect all week, then Sunday family dinner ruins everything,” she said. “Same foods, same medication, but my glucose goes crazy.”
As we talked, the pattern emerged. Every Sunday, family members would comment on her weight gain since her diabetes diagnosis. The shame would start, and her blood sugar would follow.
This shame-driven blood sugar spike is exactly what happens with self-sabotage with food—harsh self-talk triggers the same stress cascade that makes healthy choices nearly impossible.
“It’s not the Sunday potjiekos,” I realized aloud. “It’s the stress response.”
That moment changed everything – not just for Mrs. Patel, but for how I approach diabetes care in our community.
The Cortisol Timeline: When Stress Affects Blood Sugar Most
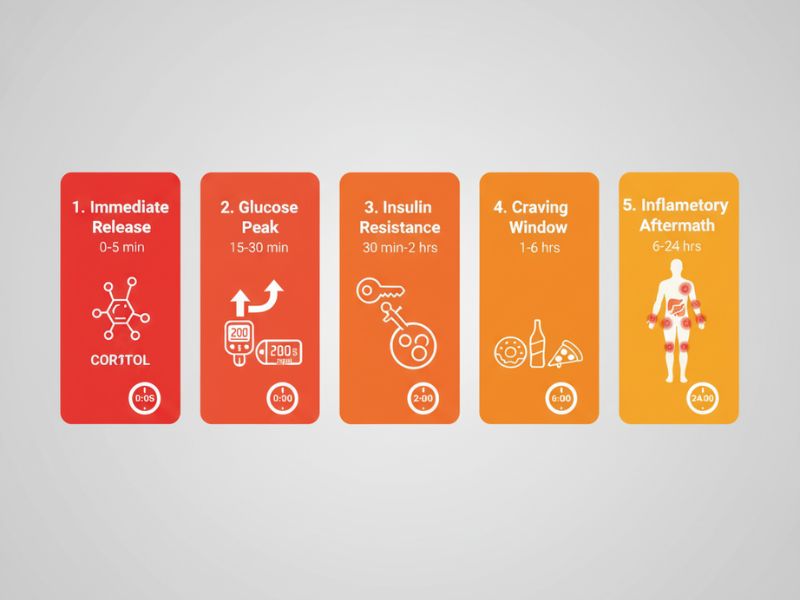
Understanding when stress affects blood sugar helps you intervene effectively:
- Immediate Release (0-5 minutes): Initially, peak cortisol hits the system
- Glucose Peak (15-30 minutes): Subsequently, blood sugar reaches its highest point
- Insulin Resistance Window (30 minutes – 2 hours): Meanwhile, the body fights its own healing
- Craving Window (1-6 hours): During this time, emotional eating impulses are strongest
- Inflammatory Aftermath (6-24 hours): Finally, body-wide inflammation affects next-day readings
In addition, this timeline explains why stress affects blood sugar for much longer than the actual stressful moment.
Breaking the Stress-Blood Sugar Cycle
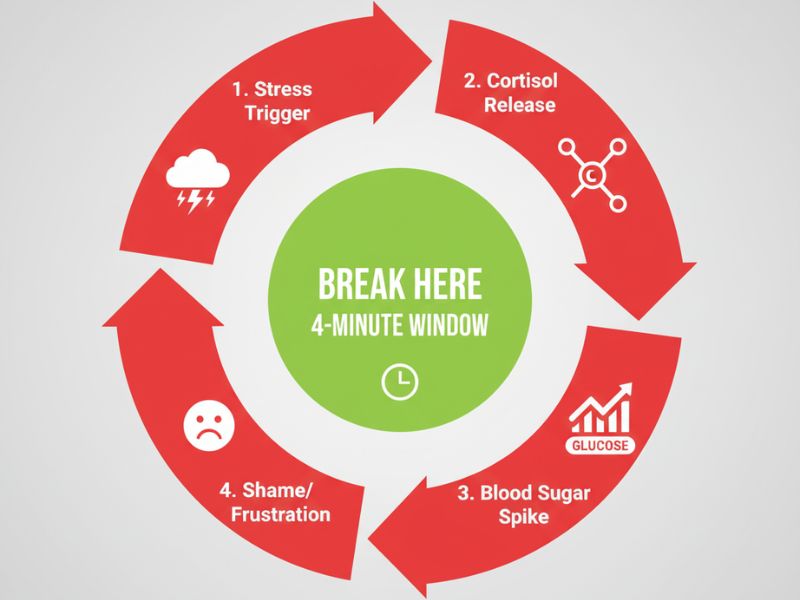
Now that you understand how stress affects blood sugar, here’s how to interrupt the process:
The 4-Minute Window
Research shows you have approximately 4 minutes from stress trigger to peak cortisol release. Master this window, and you can prevent the entire cascade.
The Immediate Response Protocol
- Recognize the stress trigger within 30 seconds
- Implement 4-7-8 breathing immediately (inhale 4, hold 7, exhale 8)
- Move your body for 60 seconds minimum
- Reframe the narrative from judgment to curiosity
Ready to break the stress-blood sugar cycle for good?
Your Body Is Talking: A Pharmacist’s Guide to Stopping Prediabetes is a free guide that explains exactly what’s happening — and what to do about it. No meal plans. No shame. Just clarity.
The Daily Prevention Strategy
Additionally, consider these daily practices:
- Morning (6-8 AM): Wake up at the same time every day to regulate natural cortisol rhythms. Eat a protein-rich breakfast within an hour of waking
- During Work Shifts: Notice when stress triggers hit (customer complaints, manager criticism). Take 60-second walking breaks during high-stress periods. Keep healthy snacks nearby for when cravings strike
- Evening (After Work): Spend 5 minutes reflecting on stress patterns from your day. Gentle stretching or a short walk to release tension. Aim for 7-8 hours of sleep to reset cortisol for tomorrow
The Stress-Blood Sugar Reality Check
Consider connecting these experiences to your own situation:
- Do the worst readings correlate with stressful periods?
- Have you noticed glucose spikes that don’t match food intake?
- Do you crave sugar most after emotional upheaval?
- Are morning readings sometimes higher despite fasting?
If you answered yes to any of these, then stress is likely affecting blood sugar more than you realize.
Many people don’t realize chronic stress patterns can contribute to insulin resistance. Learn how to recognize insulin resistance signs at home before these stress patterns compound metabolic issues.
What Changes When You Master Stress and Blood Sugar
Here’s what happens when you understand how stress affects blood sugar and take action:
- More consistent glucose readings
- Reduced unexplained spikes
- Decreased sugar cravings
- Improved insulin sensitivity
- Better sleep quality
- Enhanced emotional resilience
However, the deepest change? Finally understanding that those “random” episodes weren’t random. Instead, they were the body responding normally to abnormal internal stress.
Taking Control: From Understanding to Action

The question isn’t whether stress affects blood sugar – the science is clear. Therefore, the real question is: what will you do with this knowledge?
Every time you recognize a stress trigger, you now have 4 minutes to change the body’s biochemical response. Meanwhile, your glucose meter measures the outcome while stress awareness prevents the problem.
Now you understand how stress affects blood sugar and can take control. This isn’t just academic knowledge – it’s practical power over your health.
Ready to put this into practice? Start by tracking stress patterns alongside glucose readings for one week. You might be surprised by what you discover.
Medical Disclaimer
This blog post is for educational and informational purposes only and is not intended as medical advice. I am a licensed pharmacist sharing evidence-based health information, but I am not your healthcare provider.
If you have been diagnosed with insulin resistance, prediabetes, diabetes, or any other medical condition, consult with your doctor or qualified healthcare professional before making changes to your diet, exercise routine, or medication regimen. Individual health circumstances vary, and what works for one person may not be appropriate for another.
The information provided here is based on current scientific understanding and clinical evidence, but it does not replace personalized medical guidance from a healthcare provider who knows your complete medical history.
If you experience any concerning symptoms or have questions about your specific health situation, please seek professional medical advice.
References
- Physiology, Cortisol – StatPearls – NCBI Bookshelf. https://www.ncbi.nlm.nih.gov/books/NBK538239/
- Joseph, J.J., & Golden, S.H. (2017). Cortisol dysregulation: the bidirectional link between stress, depression, and type 2 diabetes mellitus. Annals of the New York Academy of Sciences, 1391(1), 20-34. https://doi.org/10.1111/nyas.13217
- The effect of diaphragmatic breathing on attention, negative affect and stress in healthy adults. Front Psychol. 2017;8:874.
https://doi.org/10.3389/fpsyg.2017.00874 - The Stress Axis in Obesity and Diabetes Mellitus: An Update. Endocrines, 2(3), 334-347. https://doi.org/10.3390/endocrines2030031
