
You’ve heard the word “insulin” thrown around at doctor’s appointments, seen it mentioned on health websites, maybe even had a family member diagnosed with diabetes. But do you actually know what insulin does to your body? Most people don’t. And that gap in understanding is exactly why prediabetes sneaks up on so many South Africans without warning.
I’m a pharmacist here in Cape Town, and I’ve watched too many people receive their prediabetes diagnosis with the same confused look. “But my blood sugar was fine last year,” they say. What they don’t realize is that insulin has been working overtime behind the scenes for years, slowly transitioning from hero to villain. By the time your blood sugar shows a problem, insulin resistance is already deeply established.
Today, I’m going to make insulin’s journey visible to you. Because once you understand what’s actually happening inside your body, you can stop it from progressing to Type 2 diabetes.
What Does Insulin Do to Your Body (When Everything Works)
Insulin as “The Key” That Unlocks Your Cells

Let me show you what insulin does to your body when everything is working properly.
Think of insulin as a key. Every time you eat, glucose (sugar) enters your bloodstream. But glucose can’t just float around forever—it needs to get inside your cells to create energy. That’s where insulin comes in.
Your pancreas releases insulin within minutes of eating. Insulin travels through your bloodstream until it reaches your cells, where it binds to receptors on the cell surface. This binding action is like turning a key in a lock—it opens the cell door and allows glucose to enter. Once inside, your cells convert that glucose into energy for everything you do, from walking to thinking to breathing.
After glucose enters your cells, your blood sugar levels drop back to normal. This entire process happens hundreds of times per day when your body is healthy. You never think about it. It just works.
Your Pancreas Working Behind the Scenes
Your pancreas contains specialized cells called beta cells. Their only job is to produce and release insulin. These beta cells are incredibly precise—they release exactly the right amount of insulin to match your blood sugar levels.
Eat a small apple? Your pancreas releases a small amount of insulin. Eat a plate of pap and gravy at a braai? Your pancreas releases more insulin to handle the larger glucose load.
This system works like cruise control on the N1 – it automatically adjusts to keep you at the right speed without you thinking about it. It’s automatic. Responsive. Efficient. This is insulin functioning as the hero—keeping your blood sugar balanced, your cells energized, and your body running smoothly.
What Insulin Does to Your Body When Cells Stop Listening
When Your Cells Start Ignoring the Signal

Now here’s where things start to break down. When you’re exposed to high blood sugar repeatedly—from constant snacking, processed carbs at every meal, stress-driven sugar cravings, irregular eating patterns during long retail shifts—your cells become less responsive to insulin.
It’s like the boy who cried wolf. The first time insulin shows up, cells pay attention and open their doors. The tenth time? They still respond. The hundredth time? The thousandth time? Eventually, your cells start ignoring the signal. The key still fits in the lock, but the lock is getting sticky. Harder to turn.
This is called insulin resistance. Your cells are resisting insulin’s message to open up and accept glucose. Understanding what insulin does to your body during this phase helps you see why standard tests miss it for years.
But here’s the critical part most people miss: your pancreas doesn’t just give up when cells stop responding. Instead, it compensates by producing MORE insulin. If one key doesn’t work, it sends ten keys. If ten don’t work, it sends a hundred.
This compensation phase can last for years. Your blood sugar stays “normal” on tests because your pancreas is working overtime, flooding your bloodstream with high levels of insulin (called hyperinsulinemia) to force those resistant cells open.
The Hidden Years Before Prediabetes Shows Up
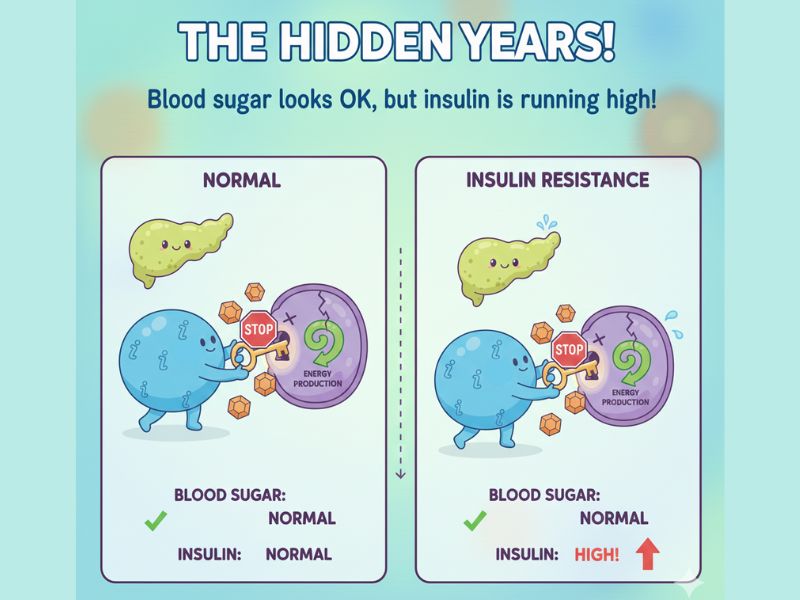
This is the invisible stage. Standard blood sugar tests look fine. You feel normal. No symptoms. Your doctor says, “Everything looks good, see you next year.”
But underneath the surface, your pancreas is exhausted, producing 2-3 times the normal amount of insulin just to maintain normal blood sugar levels. This hidden compensation phase typically lasts 5-10 years before prediabetes shows up on blood tests.
I know this pattern personally. My uncle was diagnosed with Type 2 diabetes in his 50’s. My aunt in her 40’s. When I went for a routine check-up at 34 and saw elevated cholesterol and blood pressure, my doctor said to “watch it” but my blood sugar was “normal.”
Looking back now, I understand what was happening. My body was already in the compensation phase. High insulin levels were affecting my cholesterol and blood pressure, but my blood sugar tests couldn’t detect it yet. I was years away from a prediabetes diagnosis, but the insulin resistance was already building.
What Insulin Does to Your Body When It Becomes the Villain
When High Insulin Levels Create New Problems

Once insulin resistance is established, high insulin levels start creating their own problems. This is where insulin shifts from hero to villain—not because insulin itself is bad, but because chronically elevated insulin has metabolic consequences your body wasn’t designed to handle.
What insulin does to your body changes completely when levels stay chronically elevated.
High insulin levels actively promote fat storage, especially around your belly. Insulin is a storage hormone. When your cells are already full of glucose and insulin keeps arriving with more, your body converts that excess glucose into fat and stores it. Belly fat (visceral fat) is the easiest storage location, so that’s where it accumulates first.
But here’s the vicious cycle: belly fat itself worsens insulin resistance. Fat tissue, especially visceral fat, releases inflammatory compounds that make your cells even more resistant to insulin. So now you have:
- High insulin → More belly fat
- More belly fat → Worse insulin resistance
- Worse insulin resistance → Even higher insulin needed
- Even higher insulin → More belly fat
Round and round it goes. This is why people with prediabetes often struggle with weight gain around their midsection no matter how hard they try to lose it. The insulin resistance is driving the fat storage, and the fat storage is worsening the insulin resistance.
Your Pancreas Running Out of Steam
Your pancreas can’t maintain this level of insulin production forever. Those beta cells that have been working overtime for years? They start to burn out. They become exhausted from constant overproduction.
As beta cells fail, your pancreas can’t keep up with the insulin demand anymore. That’s when blood sugar starts to rise. You’re still insulin resistant (cells still aren’t responding well), but now you also don’t have enough insulin to compensate.
This is when prediabetes finally shows up on your blood tests. Your fasting blood sugar creeps above 5.6 mmol/L. HbA1c rises above 5.7%. Your doctor delivers the diagnosis you weren’t expecting.
Without intervention at this stage, the progression continues. Beta cells keep declining. Blood sugar keeps rising. Within 3-5 years, prediabetes typically becomes Type 2 diabetes.
What Insulin Does to Your Body in Prediabetes Right Now
Why Your Doctor’s Tests Miss the Early Stages
Standard blood tests are designed to catch diabetes, not prevent it. Here’s what they actually measure:
Fasting blood sugar only shows you what’s happening after an overnight fast. It misses the insulin spikes happening throughout your day. By the time fasting blood sugar is elevated, you’re already in late-stage compensation or early pancreatic failure.
HbA1c shows your average blood sugar over 3 months. It’s useful for tracking trends, but it averages out the spikes and crashes. You can have significant insulin resistance with normal HbA1c if your pancreas is still compensating well.
Insulin levels are rarely tested in routine check-ups, even though this is where the problem starts. High insulin with normal blood sugar is the earliest detectable sign of insulin resistance, but most doctors don’t order this test unless you specifically request it.
You can have high insulin levels and normal blood sugar for years. The standard tests are designed to catch the problem after significant damage has already occurred, not during the reversible early stages.
But your body is already showing you what insulin does to your body through these signs—you just need to know how to read them. Learn to recognize insulin resistance before your doctor’s tests catch it.
The Hopeful Truth About Reversibility
Here’s what most people don’t hear when they receive their prediabetes diagnosis: insulin resistance is reversible.
Your cells can regain their sensitivity to insulin. Your pancreas can recover its normal function—as long as the beta cells aren’t too damaged yet. The earlier you intervene, the better your chances of complete reversal.
The timeline for reversal varies by person, but research consistently shows measurable improvement within 3-6 months of consistent lifestyle changes. Younger people and those diagnosed earlier in the progression typically see faster and more complete recovery.
Your body wants to work properly again. Insulin resistance isn’t a permanent sentence. It’s a reversible metabolic state that responds to the right interventions.
The WAREHOUSE Method: Making Insulin Work FOR You Again
Now that you understand what insulin does to your body and how resistance develops, you need practical tools. I’ve created the WAREHOUSE Method—nine levers you can pull to either improve insulin sensitivity or reduce insulin demand. You don’t need to be perfect with all nine. Consistent improvement with 5-6 of these creates measurable results.

W – Watch Your Carb Timing
Instead of eating all your carbs at once (which creates massive insulin surges), space them throughout the day. Smaller, more frequent doses of carbs mean smaller insulin responses. Give your pancreas recovery time between meals instead of constant demand.
A – Activate Your Muscles Regularly
Movement makes cells insulin-sensitive again. When you use your muscles, they pull glucose out of your bloodstream without needing as much insulin. Even 10-minute walks after meals create significant improvement. Your muscles become insulin-sensitive for hours after exercise.
R – Reduce Processed Food Frequency
Processed carbs cause rapid blood sugar spikes, which trigger insulin overproduction. Whole foods release glucose more slowly, creating gentler insulin responses. You don’t need to eliminate processed foods entirely—just reduce frequency. That’s where the improvement comes from.
E – Eat Protein and Fiber First
When you eat protein and fiber before carbs, they slow down glucose absorption. This smooths out the insulin release instead of creating a sharp spike. Start your meals with vegetables, lean protein, or salad, then move to starches.
Supporting Your Body’s Natural Rhythms
H – Hydrate Consistently
Dehydration concentrates blood sugar, making your pancreas work harder. Water supports kidney function, which helps clear excess glucose. Aim for at least 2 liters daily. Consistent hydration improves insulin sensitivity measurably.
O – Optimize Your Sleep Schedule
Poor sleep worsens insulin resistance directly. One night of bad sleep can reduce insulin sensitivity by 30%. Seven to nine hours of quality sleep is non-negotiable. Consistent sleep timing matters as much as duration.
U – Understand Your Stress Response
Cortisol (your stress hormone) raises blood sugar. Chronic stress means chronic insulin demand. When you’re stressed, your body releases stored glucose to prepare for “fight or flight”—but if you’re just sitting in traffic or dealing with a difficult customer, that glucose has nowhere to go. Stress management is insulin management.
S – Space Your Meals Appropriately
Constant snacking means constant insulin elevation. Your body never gets a break. Spacing meals 3-4 hours apart gives insulin levels time to drop between eating occasions. This rest period allows cells to regain sensitivity.
E – Eliminate the Shame Spiral
Shame drives stress eating. Stress eating spikes blood sugar. High blood sugar requires more insulin. The cycle perpetuates itself. Self-compassion supports sustainable change. Your body’s signals are information, not judgment. When you stop fighting yourself, insulin management becomes significantly easier.
Ready to reverse your prediabetes before it becomes diabetes?
Your Body Is Talking: A Pharmacist’s Guide to Stopping Prediabetes is a free guide that explains exactly what’s happening — and what to do about it. No meal plans. No shame. Just clarity.
Living This in Cape Town (Making It Real for You)
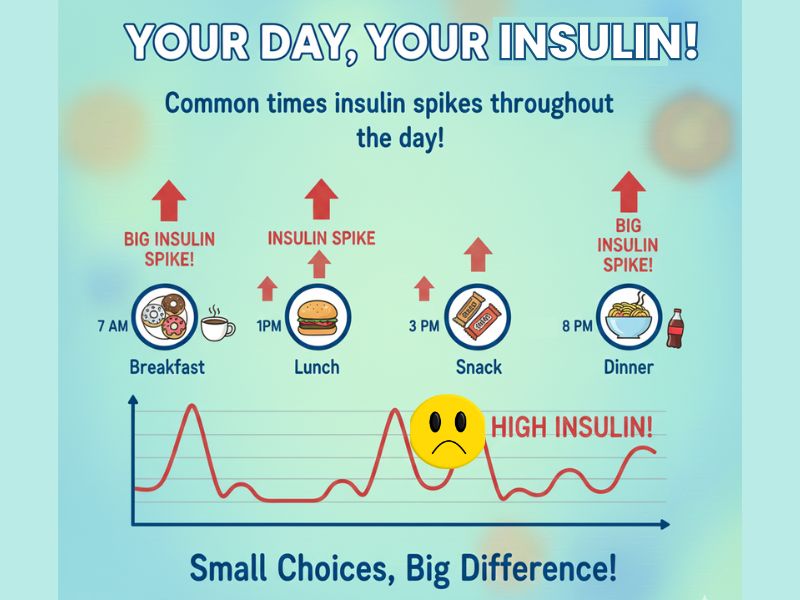
Let me show you how this plays out in real Cape Town life, because understanding the theory doesn’t help if you can’t see it in your daily routine.
You finish a long shift at Woolworths or Checkers. You’re exhausted. You grab a pre-made meal on your way out—convenient, quick, “healthy” according to the label. But even those “low fat” options are loaded with hidden carbs and sugars. Your blood sugar spikes. Insulin floods your system.
During your shift, you skipped lunch because it was busy. Now you’re eating a large meal when your body is already running on empty. Massive insulin surge. Your pancreas, which has been waiting all day, suddenly has to produce enormous amounts of insulin to handle the glucose load.
Weekend braai with friends. The social pressure to “just enjoy” makes it hard to modify your plate. Pap, potato salad, bread rolls, Castle beer—all high-carb choices that stack insulin demand on top of insulin demand. Your pancreas never gets a break.
The Convenience Trap in Cape Town Retail Life
Those Pick n Pay ready meals you buy during the week? Similar problem. “Convenient” usually means processed carbs. Your insulin levels stay elevated most of the day.
After your shift, you crack open a Castle to unwind. Your blood sugar spikes just when your insulin system is already exhausted from the day. Alcohol also impairs your liver’s ability to regulate glucose overnight, creating a double hit.
This is reality. This is the environment where insulin resistance develops. Not because you’re making “bad choices,” but because the convenient, socially acceptable options in our food culture are literally designed to spike insulin repeatedly.
Understanding what insulin does to your body means you can finally see why these patterns matter. And once you see them, you can start changing them—one meal, one choice, one WAREHOUSE principle at a time.
Your Insulin Story Isn’t Written Yet
You now understand insulin’s journey—from hero hormone unlocking your cells and maintaining balance, through the transition phase where cells start resisting and your pancreas compensates, to the villain phase where high insulin creates fat storage and vicious cycles.
But here’s the critical truth: this progression isn’t inevitable. Your insulin story isn’t finished yet.
The WAREHOUSE Method gives you nine practical levers. Each one either helps your cells regain insulin sensitivity or reduces the insulin demand on your pancreas. You don’t need perfection with all nine. Consistent improvement with 5-6 creates measurable results within 3-6 months.
The timeline reality is simple: early intervention means full reversibility is possible. Waiting years makes recovery harder—but even late intervention still brings improvement. Your doctor’s tests will eventually catch up and show the changes, but you can act now, before your diagnosis worsens.
What insulin does to your body depends on what you do with this information. Insulin isn’t the villain. Your lifestyle patterns created the resistance. And your lifestyle changes can restore the sensitivity.
The hero can return. You just have to give it the conditions it needs to work properly again.
Medical Disclaimer
This blog post is for educational and informational purposes only and is not intended as medical advice. I am a licensed pharmacist sharing evidence-based health information, but I am not your healthcare provider.
If you have been diagnosed with insulin resistance, prediabetes, diabetes, or any other medical condition, consult with your doctor or qualified healthcare professional before making changes to your diet, exercise routine, or medication regimen. Individual health circumstances vary, and what works for one person may not be appropriate for another.
The information provided here is based on current scientific understanding and clinical evidence, but it does not replace personalized medical guidance from a healthcare provider who knows your complete medical history.
If you experience any concerning symptoms or have questions about your specific health situation, please seek professional medical advice.
References
- Torjesen PA, Birkeland KI, Anderssen SA, Hjermann I, Holme I, Birkeland K. Lifestyle changes may reverse development of the insulin resistance syndrome. The Oslo Diet and Exercise Study: a randomized trial. Diabetes Care. 1997;20(1):26-31. https://diabetesjournals.org/care/article/20/1/26/18960/Lifestyle-Changes-May-Reverse-Development-of-the
- Shanik MH, Xu Y, Škrha J, Dankner R, Zick Y, Roth J. Insulin Resistance and Hyperinsulinemia: Is hyperinsulinemia the cart or the horse? Diabetes Care. 2008;31(Supplement_2):S262–S268. https://diabetesjournals.org/care/article/31/Supplement_2/S262/24841/Insulin-Resistance-and-HyperinsulinemiaIs
