
How do you lose weight if you are insulin resistant?
Your doctor says “eat less, move more.” You count calories. Join a gym. Try low-fat meal plans.
The scale drops for a few weeks. Then stops. Or worse—the weight comes back, plus extra.
Here’s what standard advice misses: when insulin resistance is driving your weight gain, “eat less, move more” doesn’t work. Not because you lack willpower. Because you’re solving the wrong problem.
As a Cape Town pharmacist with 18+ years watching this pattern repeat, I’ve seen people doing “everything right” get nowhere—and blame themselves.
The problem isn’t your effort. It’s that insulin resistance creates a metabolic trap. Your body physically cannot access stored fat for fuel when insulin levels stay elevated.
So how do you actually lose weight if you are insulin resistant?
Address insulin first. Everything else second.
Here’s how.
Why Standard Weight Loss Advice Fails When You’re Insulin Resistant
“Eat less, move more.”
It’s the advice everyone gives. And for people with normal insulin sensitivity, it works.
But when you’re insulin resistant, that advice is like telling someone with a broken leg to “just walk it off.”
I explained the three mechanisms of how insulin resistance causes weight gain in detail here: Does Insulin Resistance Cause Weight Gain?
Here’s what’s actually happening inside your body:
Normal metabolism:
- You eat → blood sugar rises → insulin released → cells absorb glucose for energy → insulin drops → body burns stored fat between meals
Insulin-resistant metabolism:
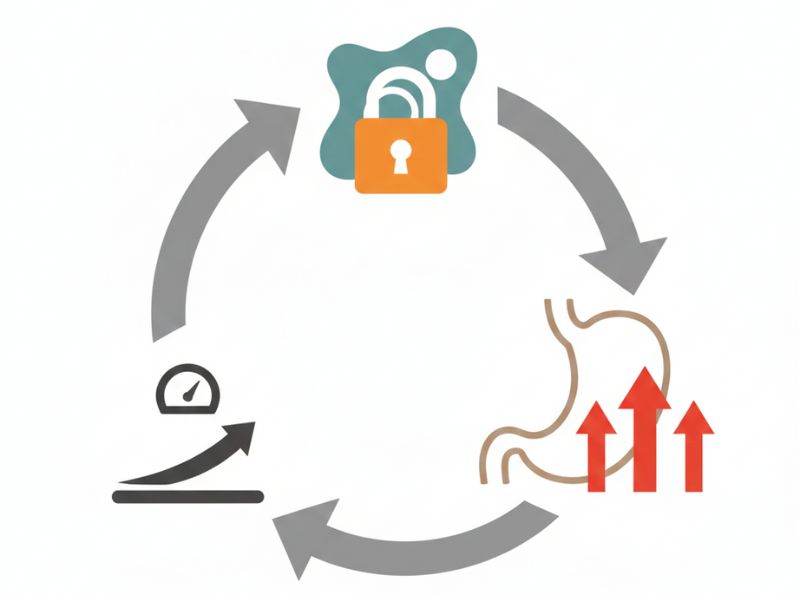
- You eat → blood sugar rises → insulin released → cells resist insulin → pancreas makes MORE insulin → glucose eventually absorbed → insulin stays elevated → body CANNOT burn stored fat
That last part is critical: high insulin levels block fat burning.
Your body literally cannot access stored fat for energy when insulin is elevated. And when you’re insulin resistant, your insulin stays elevated most of the day—even between meals.
So you cut calories. Your body needs energy. But it can’t access fat stores (insulin’s blocking it). As a result, hunger intensifies. Energy crashes. Metabolism slows down.
You’re fighting your own biology.
This is the frustration many people face. They’ve tried calorie counting, gym memberships, low-fat diets—all the standard advice.
The pattern? Temporary results that don’t last. Constant hunger. Feeling too exhausted to keep going.
The problem isn’t willpower. It’s that these approaches don’t address what’s actually driving the weight gain: insulin resistance itself.
The metabolic trap:
High insulin → can’t burn fat → stay hungry → eat to satisfy hunger → insulin spikes again → can’t burn fat → cycle continues
This is why people with insulin resistance can eat 1,200 calories per day and still not lose weight. The issue isn’t the calorie quantity. Instead, it’s metabolic access.
Your body has plenty of stored energy. It just can’t reach it.
So what’s the solution?
The answer to how to lose weight if you are insulin resistant isn’t eating less. Rather, it’s eating less frequently.
The Broken Leg vs Damaged Pancreas: Why Losing Weight With Insulin Resistance Requires Rest
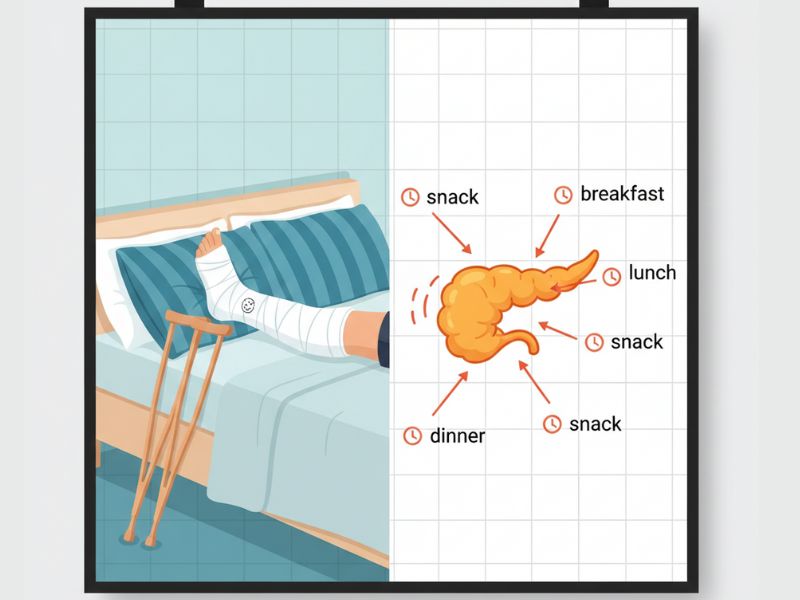
Imagine you broke your leg.
Doctor examines the X-ray. Confirms the fracture. Gives you a protocol:
“Here’s a cast. Keep weight off it for 6-8 weeks. Use crutches. Let it heal. Then we’ll start physical therapy.”
You follow the protocol. Leg heals. You’re back to normal.
Now imagine the doctor said this instead:
“Your leg is broken. You need to walk more. Try walking 10,000 steps per day. Oh, and lose some weight while you’re at it—that’ll help the healing process.”
Ridiculous, right?
You can’t heal a broken bone by forcing it to work.
Yet this is exactly what we do with damaged pancreases.
Your pancreas is overworked, inflamed, producing 2-3x normal insulin levels just to keep your blood sugar stable. It’s metabolically exhausted.
If you’re wondering whether you have insulin resistance, your body’s already telling you—here’s how to recognize the signs.
And the medical advice? “Lose weight.”
No protocol. Zero rest period. No cast.
Just: force the damaged organ to keep working overtime while simultaneously expecting it to heal.
Here’s the truth we don’t talk about: You wouldn’t run on a broken leg. So stop forcing a damaged pancreas to work 16 hours a day.
Every time you eat, your pancreas has to produce insulin. When you’re insulin resistant, it has to produce EXTRA insulin. When you eat frequently (breakfast, snack, lunch, snack, dinner, dessert), your pancreas never rests.
A broken leg gets 6-8 weeks in a cast.
Your pancreas gets… continuous work with no break.
What if we treated your pancreas like we treat broken bones?
What if we gave it a “cast”—a period of rest where it doesn’t have to produce insulin constantly?
That’s exactly what intermittent fasting does.
And just like a broken leg, healing takes time. In fact not days. Months.
But here’s what’s possible when you give your pancreas the rest it desperately needs:
- Insulin levels drop (finally allowing fat burning)
- Inflammation reduces (pancreas begins recovering)
- Cells become more sensitive to insulin again (reversal begins)
- Weight comes off naturally (not through willpower, through metabolic healing)
You’re not “going on a diet.”
You’re putting your pancreas in a cast.
How to Lose Weight If You Are Insulin Resistant: Intermittent Fasting Protocol
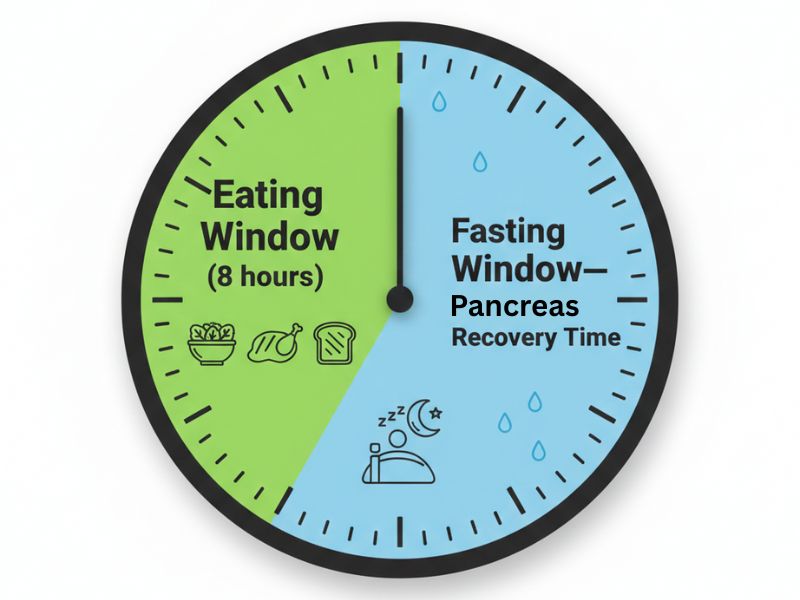
Intermittent fasting sounds complicated. However, it’s not.
It means: creating a daily window where you don’t eat, so your pancreas doesn’t have to produce insulin.
During that fasting window:
- Insulin levels drop to baseline
- Body switches from “store fat” mode to “burn fat” mode
- Pancreas rests (no insulin production needed)
- Cells begin recovering insulin sensitivity
Here’s how to lose weight if you are insulin resistant using intermittent fasting:
The protocol is simple:
Start with 12:12
12 hours not eating, 12 hours eating window.
Example: Stop eating at 7pm. Don’t eat again until 7am.
That’s it. Nothing extreme. In fact, you’re sleeping for most of it.
What this does: Gives your pancreas 12 consecutive hours without producing insulin. For many people with insulin resistance, this is the FIRST time in years their insulin levels have dropped to baseline.
Progress to 14:10 when comfortable
After 2-4 weeks of 12:12, extend the fasting window.
Example: Stop eating at 6pm. Don’t eat until 8am.
14 hours fasting, 10 hours eating.
What this does: More time for insulin to stay low. More time for your body to burn stored fat. More healing for your pancreas.
Target 16:8 as your maintenance protocol
When 14:10 feels easy, move to 16:8.
Example: Stop eating at 6pm. Don’t eat until 10am.
16 hours fasting, 8 hours eating.
This is where most insulin resistance reversal happens. Your body gets a full 16-hour fat-burning window daily. Your pancreas gets genuine rest.
What if 16:8 doesn’t work some days?
Do 14:10. Still beneficial.
Some days are harder—social events, stress, disrupted sleep. However, that’s life.
Progress over perfection.
You’re healing an organ. It doesn’t require perfection. It requires consistency over months.
What can you have during fasting?
- Water (as much as you want)
- Black coffee (no sugar, no milk)
- Plain tea (no sugar, no milk)
- Sparkling water
What breaks a fast?
Anything with calories. Milk in your coffee. A biscuit. Juice. Even “zero-calorie” sweeteners can spike insulin in some people.
If you’re hungry during the fasting window, drink water. The hunger will pass. It’s not true hunger—it’s your body adjusting to a new eating pattern.
Within 2 weeks, hunger during fasting windows typically disappears. Your body adapts.
What to Eat to Lose Weight With Insulin Resistance
Intermittent fasting gives your pancreas rest.
But what you eat during your eating window determines how MUCH insulin your pancreas has to produce when it’s working.
This is the second part of how to lose weight if you are insulin resistant—not just when you eat, but what you eat.
The goal: eat foods that require minimal insulin response.
Therefore, here’s the framework:
Protein first
Protein stabilizes blood sugar and increases satiety (you feel full longer).
Examples:
- Eggs
- Chicken
- Fish
- Beef
- Lamb
- Greek yoghurt (full-fat, no added sugar)
Aim for 25-35 grams of protein per meal. That’s roughly the size of your palm.
Fiber second
Fiber slows glucose absorption, preventing blood sugar spikes.
Examples:
- Vegetables (especially leafy greens, broccoli, cauliflower)
- Legumes (lentils, beans)
- Berries
- Avocado
Fill half your plate with vegetables. In fact, this is non-negotiable.
Healthy fats third
Fats satisfy hunger and don’t spike insulin.
Examples:
- Olive oil
- Avocado
- Nuts (almonds, macadamias, walnuts)
- Seeds (chia, flax, pumpkin)
- Butter (real butter, not margarine)
Don’t fear fat. After all, fat doesn’t make you fat when insulin is controlled. High insulin makes you fat.
What to minimize
These spike insulin significantly:
- White bread, rolls, wraps
- Rice, pasta, potatoes
- Sugary drinks (cold drinks, fruit juice, sweetened coffee)
- Sweets, biscuits, cakes
- Processed snacks (chips, crackers)
You don’t have to eliminate them forever. However, while healing insulin resistance, minimize them. Once your insulin sensitivity improves (3-6 months), you’ll have more metabolic flexibility.
Sample day:
10am (break fast):
- 3-egg omelette with spinach, tomato, mushrooms
- Half an avocado
- Black coffee or tea
2pm (lunch):
- Grilled chicken on mixed salad (lettuce, cucumber, peppers, onion)
- Olive oil and vinegar dressing
- Handful of nuts
6pm (dinner, then start fast):
- Grilled fish or beef
- Roasted vegetables (broccoli, cauliflower, butternut)
- Small portion sweet potato (if desired)
Notice: No snacks. Instead, three meals during the 8-hour window, then done.
This isn’t starvation. It’s strategic eating that keeps insulin low most of the day.
For more info, read about Foods to Reverse Prediabetes: A Pharmacist’s Guide.
The Shame-Free Approach to Insulin Resistance Weight Loss
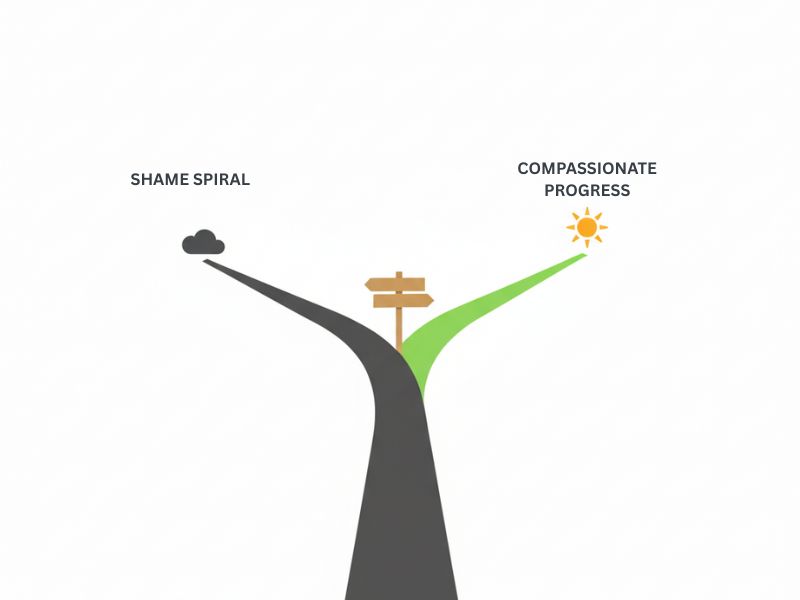
Here’s something most weight loss advice won’t tell you:
Shame worsens insulin resistance.
When you feel ashamed—about your weight, your choices, your “failure” to stick to a diet—your body releases cortisol (stress hormone).
High blood sugar triggers insulin release.
More insulin worsens insulin resistance.
Shame literally makes your condition worse.
So here’s the approach that actually works:
Progress over perfection.
Some days you’ll hit 16:8 easily. Other days you’ll barely manage 12:12. Both are beneficial.
Start with 12:12.
Most people already fast 8-10 hours overnight without thinking about it. You’re just extending it slightly.
Progress when comfortable.
After 2-4 weeks of 12:12, try 14:10. When that feels easy, try 16:8.
16:8 not working today?
Do 14:10. Still beneficial.
Life happens. Social events. Family gatherings. Stressful workdays. Some days you’ll break your fast earlier. That’s fine.
You’re not failing. You’re living.
One “off” day doesn’t erase progress.
If you break your eating window on Saturday, start fresh on Sunday. Don’t spiral into “I’ve already ruined it, might as well eat whatever.”
That’s shame talking. Ignore it.
You’re healing an organ, not testing willpower.
This isn’t about discipline or self-control. It’s about giving your pancreas the rest it needs to recover.
Some days it gets more rest. Some days less. Over weeks and months, the cumulative rest adds up.
What you do consistently matters more than doing it perfectly.
Supporting Your Insulin Resistance Weight Loss: Sleep, Stress, Movement
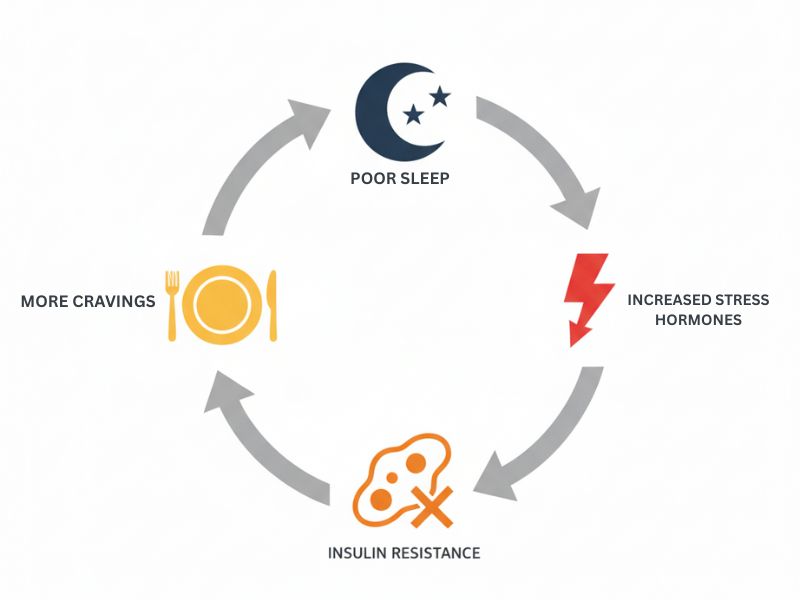
Intermittent fasting is the foundation. But three other factors significantly impact insulin sensitivity:
Sleep (7-9 hours nightly)
Poor sleep wrecks insulin sensitivity.
One night of bad sleep can reduce insulin sensitivity by 30%. Furthermore, chronic poor sleep keeps insulin resistance locked in place.
Why? Sleep deprivation increases cortisol. Cortisol raises blood sugar. High blood sugar requires more insulin.
Target: 7-9 hours per night, consistently.
If you’re only sleeping 5-6 hours, improving sleep alone can accelerate insulin resistance reversal by months.
Stress management
Chronic stress = chronically elevated cortisol = chronically elevated blood sugar = chronically elevated insulin.
You can fast perfectly and eat perfectly, but if you’re drowning in stress, your insulin resistance won’t improve.
Therefore, practical stress reduction:
- Walk outside daily (20-30 minutes, no phone)
- Deep breathing (5 minutes when overwhelmed)
- Time in nature (even a park helps)
- Say no more often (retail managers especially—you can’t fix every crisis)
You’re not “adding self-care.” You’re removing insulin-spiking cortisol from your system.
Movement (especially after meals)
Here’s something remarkable: muscle uses glucose without requiring insulin.
When you move, your muscles pull glucose directly from your bloodstream. No insulin needed.
This means walking after meals:
- Lowers blood sugar naturally
- Reduces insulin demand on your pancreas
- Improves insulin sensitivity over time
You don’t need a gym membership.
A 10-15 minute walk after dinner is enough. Around the block. In your neighbourhood. At the mall before driving home.
Consistency beats intensity.
Strength training 2x per week also helps (muscle tissue improves insulin sensitivity), but walking after meals is the easiest, most sustainable habit.
These three support fasting. However, they don’t replace it.
You can’t out-sleep poor eating habits.
You can’t out-walk insulin resistance without addressing meal timing.
Intermittent fasting creates the foundation—sleep, stress management, and movement accelerate progress from there.
Insulin Resistance Weight Loss Timeline: What to Expect
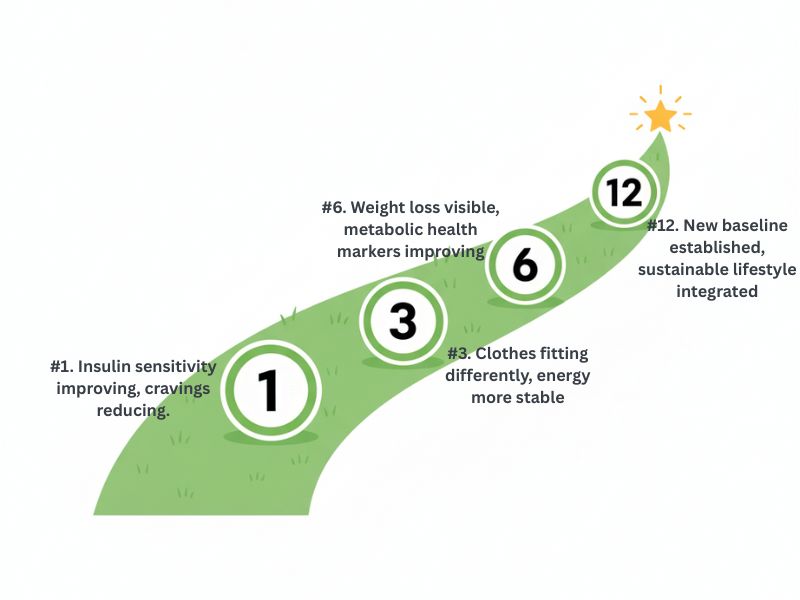
Healing insulin resistance takes time. Here’s what the research shows:
Week 1-2: Adjustment Period
Your body is adapting to a new eating pattern.
What you might feel:
- Hunger during fasting windows (usually passes by week 2)
- Slight energy dips (temporary, as body learns to burn fat)
- Irritability (blood sugar stabilizing)
What’s actually happening:
- Insulin levels beginning to drop
- Body switching from constant glucose-burning to fat-burning
- Pancreas getting first real rest in years
Don’t quit here. This phase is temporary. Most people feel dramatically better by week 3.
Month 1: Early Wins
What you’ll notice:
- Clothes fit differently (especially around waist)
- Less bloating
- Mental clarity improving (no more afternoon fog)
- Energy stabilizing (no more 3pm crashes)
- Scale might show 2-4 kilograms down
What’s happening internally:
- Inflammation reducing
- Insulin levels lower throughout the day
- Cells beginning to respond to insulin again
- Fasting blood glucose dropping (might go from 6.5 mmol/L to 6.0 mmol/L)
Month 3: Measurable Improvement
What you’ll notice:
- Weight loss visible (friends commenting)
- Energy consistently better
- Hunger patterns completely changed (no longer thinking about food constantly)
- Sleep quality improved
- Scale shows 5-8 kilograms down
What’s happening internally:
- Insulin sensitivity measurably improving
- Fasting blood glucose potentially down to 5.5-5.8 mmol/L
- HbA1c dropping (might go from 6.2% to 5.9%)
- Pancreas recovering function
Month 6-12: Reversal Zone
What you’ll notice:
- Weight loss sustained (10-15+ kilograms down, depending on starting point)
- 16:8 feels natural (no longer “fasting,” just how you eat)
- Metabolic flexibility returning (can occasionally eat carbs without crashes)
- Medical markers improving (doctor notices)
What’s happening internally:
- Insulin sensitivity significantly improved or normalized
- Fasting blood glucose potentially in normal range (under 5.6 mmol/L)
- HbA1c potentially reversed out of prediabetic range (under 5.7%)
- Pancreas function restored
This is what successful weight loss with insulin resistance looks like—not through restriction, but through metabolic healing.
Your actual timeline might look something like this:
Month 1: Lost 3 kilograms, energy better, less brain fog Month 3: Down 7 kilograms total, fasting glucose from 6.4 to 5.9 mmol/L Month 6: Down 12 kilograms, HbA1c from 6.1% to 5.6% (no longer prediabetic)
Not dramatic overnight transformation. Steady, sustainable healing.
Important: Your timeline might differ. Some people see faster results. Others slower. Age, starting weight, how long you’ve been insulin resistant, sleep quality, stress levels—all impact speed of reversal.
But the direction is consistent: give your pancreas rest, insulin sensitivity improves, weight comes off naturally.
Conclusion:

Your doctor said, “Lose weight.”
But didn’t give you the protocol for HOW when your metabolism is broken.
Now you have it:
The cast your pancreas needs: Intermittent fasting (start 12:12, progress to 16:8)
What to eat: Protein first, fiber second, healthy fats third. Minimize refined carbs.
Supporting pillars: 7-9 hours sleep, stress management, walk after meals
Timeline: 3-6 months for measurable improvement, 6-12 months for potential reversal
This isn’t a quick fix. It’s a healing protocol.
You’re not “going on a diet.” You’re treating insulin resistance at its source—giving your pancreas the rest it’s been begging for.
Others did this. Their colleagues noticed at month 2. Their doctors were impressed at month 6. They are no longer prediabetic.
You can do this too.
Not through willpower. Through understanding how your body actually works and working with it, not against it.
Your broken leg gets a cast. A damaged pancreas deserves one too.
Your Body Is Talking: A Pharmacist’s Guide to Stopping Prediabetes is a free guide that explains exactly what’s happening — and what to do about it. No meal plans. No shame. Just clarity.
Medical Disclaimer
This blog post is for educational and informational purposes only and is not intended as medical advice. I am a licensed pharmacist sharing evidence-based information about insulin resistance and weight management, but I am not your healthcare provider.
If you have been diagnosed with insulin resistance, prediabetes, diabetes, or any other medical condition, consult with your doctor or qualified healthcare professional before making changes to your diet, exercise routine, or medication regimen. Individual health circumstances vary, and what works for one person may not be appropriate for another.
The information provided here is based on current scientific understanding and clinical evidence, but it does not replace personalized medical guidance from a healthcare provider who knows your complete medical history.
If you experience any concerning symptoms or have questions about your specific health situation, please seek professional medical advice.
References:
1: Sutton EF, Beyl R, Early KS, Cefalu WT, Ravussin E, Peterson CM. Early Time-Restricted Feeding Improves Insulin Sensitivity, Blood Pressure, and Oxidative Stress Even Without Weight Loss in Men with Prediabetes. Cell Metabolism. 2018;27(6):1212-1221. https://pmc.ncbi.nlm.nih.gov/articles/PMC5990470/
2: Yuan X, Wang J, Yang S, Gao M, Cao L, Li X, Hong D, Tian S, Sun C. Effect of Intermittent Fasting Diet on Glucose and Lipid Metabolism and Insulin Resistance in Patients with Impaired Glucose and Lipid Metabolism: A Systematic Review and Meta-Analysis. Int J Environ Res Public Health. 2022;19(6):3341. https://pmc.ncbi.nlm.nih.gov/articles/PMC8970877/
