
Does lack of sleep affect blood sugar levels?
Before I answer, I want to tell you about someone I spoke to recently.
She is insulin resistant. Has been told she has “stage 1 diabetes” — which is most likely prediabetes, just described in different language by a different doctor. She is doing her best — she is trying. And her sleep is being destroyed every night by something completely outside her control — a neighbor living with dementia, whose nights have no pattern, no quiet, and no mercy.
She is not failing at sleep. Life is happening to her.
And her blood sugar is paying the price. If you have ever wondered whether lack of sleep affects blood sugar levels — the answer is yes. And her story is exactly why that matters.
Does Lack of Sleep Affect Blood Sugar Levels? The Short Answer
Yes. Significantly.
A single night of poor sleep is enough to impair your body’s ability to manage glucose the following day. Research published in journals including Diabetes Care and the Annals of Internal Medicine has consistently shown that sleep deprivation reduces insulin sensitivity — sometimes to a degree comparable to eating a high-sugar diet for several weeks.
That is not a small effect. That is your body, after one bad night, struggling to do what it normally does without effort.
However, understanding why this happens is more useful than just knowing that it does. Because when you understand the mechanism, you stop blaming yourself — and you start working with your biology instead of against it.
Important before you continue: Sleep deprivation affects how your body manages glucose — and if you are on insulin, sulfonylureas, or blood pressure medication, disrupted sleep can interact with how those medications work. If you are managing prediabetes with medication, speak to your pharmacist or doctor before making any changes to your routine. If you are on Metformin only, your risk is lower — but the conversation is still worthwhile.
How Lack of Sleep Affects Blood Sugar Levels
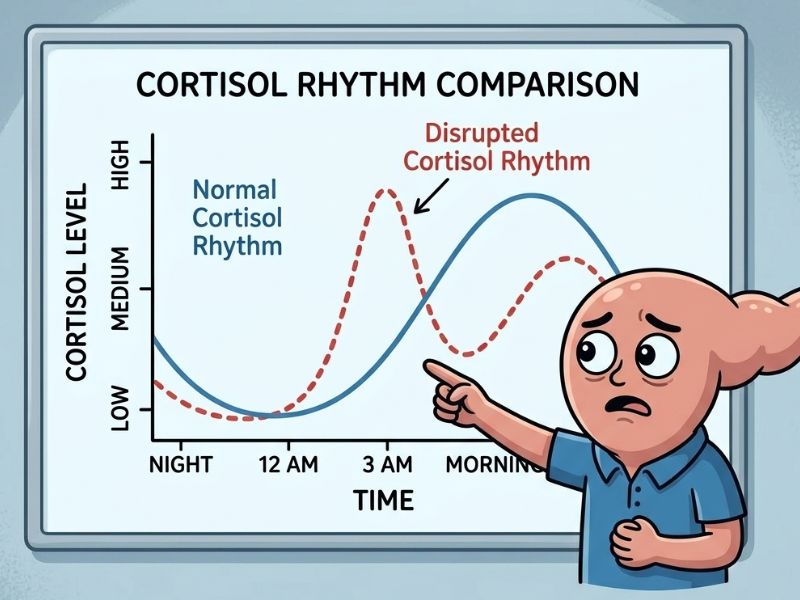
When you do not get enough sleep, two hormones rise that your body would normally keep in check overnight: cortisol and growth hormone.
Cortisol is your stress hormone. In a well-rested body, cortisol follows a natural rhythm — low at night, rising gradually toward morning to prepare you for the day. When sleep is disrupted, that rhythm breaks down. Cortisol spikes at the wrong time, triggering your liver to release stored glucose into your bloodstream. Your blood sugar rises — not because you ate anything, but because your stress system activated.
Growth hormone, which is normally released during deep sleep, helps repair tissues overnight. As part of this process, it creates a brief, intentional window of insulin resistance in the early morning hours — your body temporarily prioritising repair over glucose uptake. This is normal physiology. However, when sleep is fragmented, the growth hormone pulse is disrupted and the cortisol rhythm breaks down alongside it. The dominant driver of the prolonged insulin resistance you feel after a bad night is not growth hormone — it is elevated cortisol combined with an overactive sympathetic nervous system, your body stuck in “awake” mode when it should be resting.
Consequently, you wake up with elevated blood sugar, reduced insulin sensitivity, and a body that is already on the back foot before the day has even started.
Furthermore, sleep deprivation increases levels of ghrelin — the hunger hormone — while reducing leptin, which signals fullness. As a result, you are not only managing higher blood sugar the morning after a bad night. You are also hungrier, more likely to reach for fast energy (sugar, refined carbs), and less equipped neurologically to make the calm, considered choices that support your health.
This is not weakness. This is biology.

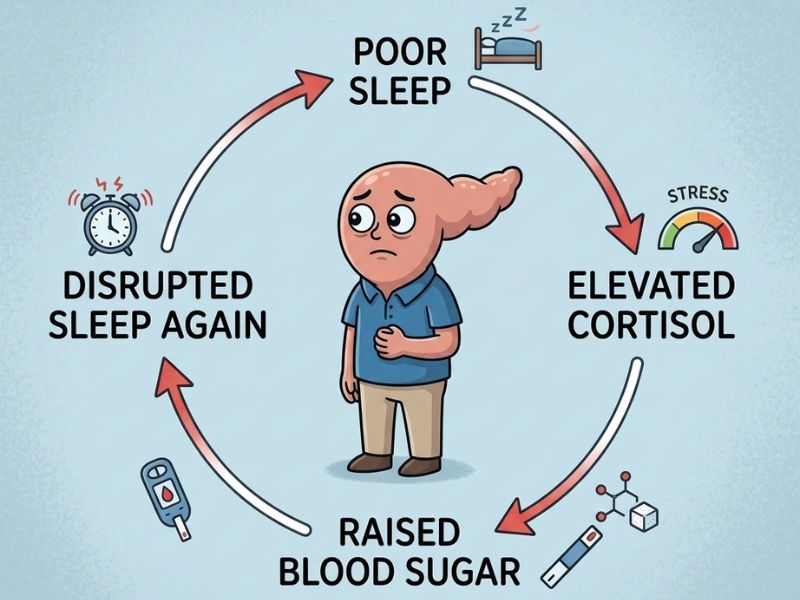
Lack of Sleep and Blood Sugar — The Cruel Loop
Here is where it becomes important to name something clearly.
Poor sleep raises blood sugar. Elevated blood sugar — particularly in the context of insulin resistance — can disrupt sleep quality. The two feed each other. Therefore, if you are already dealing with prediabetes, disrupted sleep is not just a side issue. It is a direct metabolic problem sitting inside the same loop you are trying to break.
High blood sugar can cause increased thirst and more frequent urination at night — both of which fragment sleep further. Similarly, the cortisol dysregulation that comes with insulin resistance can make it harder to stay asleep even when the external environment is quiet.
In other words: your prediabetes may be making your sleep worse, and your poor sleep is making your prediabetes worse.
That is the cruel loop. And the person I described at the beginning of this blog — she is living inside it, through no fault of her own.
If you want to understand the full picture of what is driving your blood sugar — not just sleep, but stress, food, movement, and the patterns underneath all of it — the free ebook covers all of it in one place.
When the Cause Is Outside Your Control
This is the part that most sleep advice skips entirely.
“Get eight hours.” “Improve your sleep hygiene.” “Go to bed at the same time every night.”
That advice assumes the problem is a habit. It assumes you are choosing poor sleep. It assumes that if you just tried harder, or downloaded the right app, or turned your phone off earlier, the problem would resolve.

But what about the neighbor with dementia whose distress has no schedule? What about the shift worker whose roster changes every week? What about the parent of a sick child, the person in a difficult living situation, the man working two jobs whose body never fully rests?
Standard sleep advice is useless to these people — not because they are not trying, but because the source of the disruption is outside their control.
As a pharmacist with nearly two decades of experience, I have seen what shame does to people in this position. They already know they are not sleeping well. Telling them to sleep better without acknowledging why they cannot is not helpful. It is demoralising.
So let us talk about what is actually in your control when the sleep itself is not.
Managing Blood Sugar Levels When Sleep Is Disrupted
You cannot always fix the disruption. However, you can change how your body responds to it. These are not tips for perfect conditions — these are strategies for real life.
1. Anchor your morning regardless of how the night went

A short walk after waking — even ten minutes — activates your muscles to take up glucose independently of insulin. Furthermore, it begins to bring cortisol back into its natural rhythm. You are not undoing the bad night. You are giving your body the best possible starting point for the day that follows it. For more on how movement timing affects your glucose response, Walking After Eating: 15 Minutes That Lower Blood Sugar explains why that post-waking walk works the way it does.
2. Prioritise protein at your first meal

After a disrupted night, your hunger hormones are working against you. Consequently, a carb-heavy breakfast — even a seemingly healthy one — is likely to spike your blood sugar in a body that is already insulin resistant from the night before. Protein slows digestion, blunts the glucose response, and keeps you fuller for longer without the spike. Think two scrambled eggs with spinach, or Greek yoghurt with berries and a handful of nuts.
3. Notice — do not judge — the cravings
Sleep deprivation will make you want sugar. That is not a character flaw. That is ghrelin doing exactly what it is designed to do. Recognising the craving as a hormonal signal rather than a moral failure changes your relationship to it — and if you want to understand the cortisol layer underneath that craving, Cortisol Sugar Cravings unpacks exactly why stress and poor sleep send you reaching for the same things. You do not have to obey the craving. But you do not have to shame yourself for having it either.
4. Reduce other stressors where possible
Your cortisol bucket is already fuller than usual after a bad night. Therefore, anything that adds to it — an argument, a skipped meal, a high-intensity workout when your body is exhausted — will compound the blood sugar effect. This is not an excuse to do nothing. It is a reason to be strategic. A gentle walk is better than a hard gym session on three hours of sleep. A regular meal is better than extended fasting when your stress hormones are already elevated. If you want to understand how stress drives blood sugar independently of sleep, Does Stress Affect Blood Sugar? The Hidden Truth covers the full mechanism.
5. Let sleep debt repay itself gradually
You cannot catch up on a week of poor sleep in one long Saturday morning. However, consistently protecting even one or two better nights per week begins to restore insulin sensitivity over time. Progress is not linear. But every recovered night is doing real metabolic work.
Lack of Sleep and Insulin Resistance — The Bigger Picture
Sleep is not a lifestyle luxury. It is a metabolic necessity. And if you are still asking does lack of sleep affect blood sugar levels — the research is unambiguous: yes — chronically and significantly.
Every major system that governs your blood sugar — cortisol regulation, insulin sensitivity, hunger signalling, glucose uptake — is actively managed during sleep. When sleep is disrupted chronically, these systems do not just underperform the next day. They begin to recalibrate around a new, lower baseline.
This is why research consistently links chronic sleep deprivation to the progression of prediabetes to Type 2 diabetes. It is not simply that tired people make worse food choices — though that is also true. It is that the sleep deprivation itself is driving insulin resistance at a biological level.
Furthermore, the people most affected by chronic poor sleep are often the same people already carrying the highest metabolic burden — shift workers, caregivers, people in difficult life circumstances, people under prolonged stress. The overlap is not coincidence.
And if you are looking for a strategy that works alongside better sleep to actively lower your blood sugar — not just protect against a bad night — Does Fasting Lower Blood Sugar Levels? A Pharmacist Explains is worth reading next.
The Awareness Layer — What You Can Control

Here is what I want to leave you with.
You cannot control your neighbor’s dementia. Nor can you control a shift roster. You cannot control a child who needs you at 3 AM.
But you can choose how you respond to what follows. Before you reach for sugar, ask what your body actually needs. Before you judge yourself for the exhaustion, remember that your body is responding to circumstances — not failing because of weakness.
That moment of awareness — small as it sounds — is the beginning of working with your biology instead of fighting it. It is the difference between a bad night becoming a bad day, and a bad night being exactly what it was: one difficult night that your body can recover from, given the right conditions.
She is not failing. You are not failing either. The body is responding to circumstances. And circumstances — even the ones outside your control — can be navigated with the right information.
That is what this is for.
The Bottom Line
Does lack of sleep affect blood sugar levels? Yes — through cortisol dysregulation, reduced insulin sensitivity, and disrupted hunger hormones. One bad night is enough to create measurable metabolic impact.
However, when the cause of that poor sleep is outside your control, the answer is not better sleep hygiene. The answer is understanding what is happening in your body, reducing the downstream damage where you can, and removing the shame from a situation that was never your fault to begin with.
If you are managing prediabetes in difficult circumstances — if life is happening to you — this blog was written for you specifically.
The free ebook walks you through the complete Helping Prediabetics framework — nutrition, movement, sleep, stress, and the awareness layer that ties it all together. It is free. And it was written for exactly the person described in this blog.
References
- Spiegel K, Leproult R, Van Cauter E. Impact of sleep debt on metabolic and endocrine function. Lancet. 1999;354(9188):1435–1439. https://pubmed.ncbi.nlm.nih.gov/10543671/
- Donga E, van Dijk M, van Dijk JG, et al. A single night of partial sleep deprivation induces insulin resistance in multiple metabolic pathways in healthy subjects. Journal of Clinical Endocrinology & Metabolism. 2010;95(6):2963–2968. https://pubmed.ncbi.nlm.nih.gov/20371664/
- Cappuccio FP, D’Elia L, Strazzullo P, Miller MA. Quantity and quality of sleep and incidence of type 2 diabetes. Diabetes Care. 2010;33(2):414–420. https://pubmed.ncbi.nlm.nih.gov/19910503/
