
You’re eating healthy and exercising. You’re doing everything “right”—but the scale won’t budge. Maybe it’s even climbing despite your best efforts. Then your doctor mentions insulin resistance during a routine visit. Suddenly you’re wondering: does insulin resistance cause weight gain? Is this why I can’t lose weight?
The short answer is yes. Insulin resistance makes weight loss significantly harder by trapping fat inside your cells, driving relentless hunger, and slowing your metabolism. But here’s what matters more than the “yes”—understanding how insulin resistance causes weight gain gives you power to reverse it.
I’m a Cape Town pharmacist with 18+ years helping people navigate prediabetes. I’ve seen this pattern hundreds of times: people doing what their doctor recommended, but insulin resistance working against them the entire time. Here’s what’s actually happening in your body—and what helps.
In this post, I’ll walk you through the biological mechanism linking insulin resistance to stubborn weight gain, explain why traditional “eat less, move more” advice often fails when insulin resistance is present, and show you what actually works instead.
What Insulin Resistance Does to Your Body and Weight

Let’s start with a quick recap from my previous post about what insulin does to your body. Think of insulin as a key. When you eat, your blood sugar rises, and your pancreas releases insulin. That insulin acts like a key that unlocks your cells so glucose can enter and be stored for energy. Simple. Effective. That’s how it’s supposed to work.
But with insulin resistance, your cells stop responding to insulin’s signal. They’ve become “resistant” to the key. So your pancreas compensates by producing more insulin—turning up the volume, essentially, to get the same message across. Now you need higher levels of insulin just to do the same job that normal amounts used to handle.
Here’s where the problem compounds. High insulin levels actively promote fat storage. And the more fat you store (especially around your midsection), the more insulin resistant you become. Which means your pancreas has to produce even more insulin. You’re trapped in a vicious cycle: high insulin causes more fat storage, which worsens insulin resistance, which drives insulin even higher.
This matters tremendously for weight because insulin is fundamentally a storage hormone. When insulin is elevated in your bloodstream, your body stays locked in “store mode” instead of “burn mode.” You literally cannot access your own stored fat for energy while insulin levels remain high.
So, does insulin resistance cause weight gain? Absolutely—and here’s exactly how it happens.
The Three Ways Insulin Resistance Causes Weight Gain
Let me break down exactly the three mechanisms showing how insulin resistance causes weight gain and makes weight loss feel impossible.
Insulin Blocks Fat Burning
When insulin is high, your body cannot access stored fat for energy. Period. It’s like having a savings account you’re not allowed to withdraw from. The fat is there—often plenty of it—but insulin blocks the enzymes needed to break it down and use it for fuel.
This means even when you’re restricting calories and exercising, even when you’re genuinely creating an energy deficit, your body still can’t tap into fat stores efficiently. High insulin keeps that fat locked away. Instead, your body burns through whatever glucose is available and then signals desperately for more food because it thinks it’s starving.
This is why people with insulin resistance say things like “I’m eating 1,200 calories a day and I’m still not losing weight.” They’re not lying. They’re not miscounting. Their bodies are genuinely unable to access stored energy because insulin resistance has essentially locked them out of their own fuel reserves.
Insulin Drives Hunger and Cravings

Here’s the second mechanism. When insulin is chronically elevated, it tends to drive blood sugar down—sometimes rapidly. Your body interprets dropping blood sugar as a crisis signal. Suddenly you’re intensely hungry even though you just ate two hours ago.
Your brain receives the message that energy is scarce and responds with overwhelming cravings, usually for quick energy sources like carbohydrates and sugar. These aren’t psychological cravings you can overcome with willpower. These are biological survival signals your body is screaming at you.
So you eat. The carbs spike your blood sugar. Your insulin surges to handle it. The cycle repeats. Meanwhile, you feel like you lack discipline or self-control when really your body’s signaling system is completely disrupted. Willpower isn’t the problem—your biology is working against you.
Insulin Disrupts Your Metabolism
The third way insulin resistance causes weight gain is by gradually slowing your metabolic rate. When your body is constantly dealing with high insulin levels, it adapts. It becomes more efficient at storing energy and less efficient at burning it.
This is the phenomenon researchers call “metabolic adaptation.” Your body literally burns fewer calories at rest and during activity than it should based on your weight and muscle mass. It’s protecting itself against what it perceives as chronic energy scarcity—even though you’re eating normally or even restricting calories.
This is why the classic “eat less, move more” approach eventually stops working for people with insulin resistance. You cut calories. You lose a bit of weight initially. Then your metabolism slows to match your reduced intake. The weight loss stalls. You cut calories further. Your metabolism slows again. You’re caught in a race to the bottom that you cannot win because you’re not addressing the underlying insulin problem.
Why You Gained Weight in the First Place
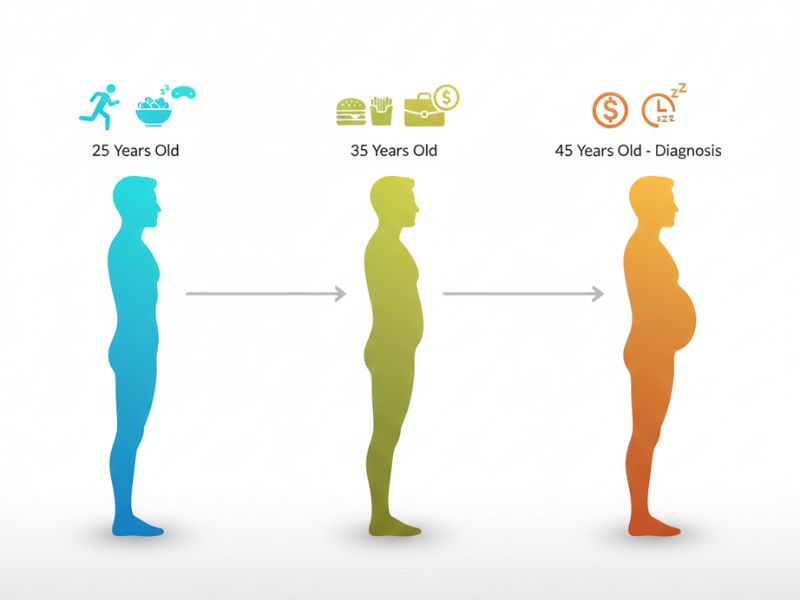
If you’re reading this and recognizing yourself in these descriptions, you might be wondering how you ended up here. Insulin resistance doesn’t develop overnight. It’s a gradual process that typically unfolds over years, often starting in your 20s or 30s.
You probably missed the early warning signs. Maybe you noticed your energy crashing in the afternoon. Or, maybe you started accumulating fat around your midsection even though your arms and legs stayed relatively lean. Maybe you found yourself getting hungry again shortly after meals, especially meals high in carbohydrates.
The typical progression looks something like this: You maintain a normal weight through your 20’s. Then you start noticing gradual weight gain, especially around your middle. You try the usual strategies—cutting calories, adding cardio—and they work less effectively than they used to. Eventually those strategies stop working entirely. You get frustrated. Your doctor runs tests and discovers elevated fasting insulin or impaired glucose tolerance or both. That’s when you hear the words “insulin resistance” or “prediabetes.”
Now you understand that insulin resistance does cause weight gain through specific hormonal mechanisms, not lack of willpower.
Also, what’s critical to understand is that this isn’t about a lack of discipline either. This is hormonal dysfunction. Your body’s signaling system broke down gradually over time, driven by factors like processed food consumption, chronic stress, poor sleep, and sedentary lifestyle. But the mechanism driving your weight gain is biological, not behavioral.
Can You Lose Weight When Insulin Resistance Causes Weight Gain?

Here’s the question I know you’re really asking: does insulin resistance cause weight gain, and can you actually lose weight despite it?
Yes, you can lose weight even when insulin resistance causes weight gain—but not by traditional methods alone.
You cannot successfully lose weight long-term by simply eating less and moving more when insulin resistance is present. You’ve probably already discovered this the hard way. What you must do instead is address the insulin resistance itself.
When insulin sensitivity improves—when your cells start responding normally to insulin again—weight loss becomes possible. Not just possible, but almost automatic. As insulin levels drop back to normal ranges, your body can finally access stored fat for energy. The constant hunger signals quiet down. Your metabolism stops suppressing itself.
Real-world evidence backs this up consistently. People who successfully reverse insulin resistance through dietary and lifestyle changes typically lose 5-10% of their body weight naturally without aggressive calorie restriction. The weight comes off because the hormonal dysfunction causing weight gain has been corrected.
What Actually Works

So what does addressing insulin resistance actually look like? The core principle is simple: you must lower insulin levels, not just calories.
The Five Key Strategies
Start by reducing refined carbohydrates and added sugars. These foods spike blood sugar and require massive insulin responses. When you minimize them, you give your pancreas a break and allow insulin levels to drop. This doesn’t mean zero carbs forever—it means prioritizing whole foods over processed ones and being strategic about when and how much carbohydrate you consume.
Learn more about which foods help lower insulin naturally in my guide to foods that reverse prediabetes.
Increase protein and fiber with every meal. Both slow digestion and create more stable blood sugar responses. This means smaller insulin spikes, which over time helps improve insulin sensitivity. Aim for a palm-sized portion of protein and at least one serving of non-starchy vegetables with each meal.
Add strength training to your routine. Muscle tissue is highly insulin-sensitive. When you build muscle, you create more places for glucose to go that respond well to insulin. You don’t need to become a bodybuilder—even two to three sessions per week of basic resistance training makes a measurable difference.
Manage stress and prioritize sleep. Cortisol, your primary stress hormone, directly interferes with insulin signaling. Chronic stress and poor sleep both elevate cortisol and worsen insulin resistance. This isn’t optional self-care—it’s metabolic medicine.
Discover exactly how stress affects your blood sugar and insulin sensitivity in my detailed breakdown.
Consider intermittent fasting or time-restricted eating. When you extend the time between meals, insulin levels naturally drop during the fasting period. This gives your body regular breaks from elevated insulin and improves insulin sensitivity over time. Start simple—perhaps a 12-hour overnight fast—and adjust based on how you feel.
Why This Works Differently
What makes this approach different from conventional dieting is that you’re fixing the underlying mechanism instead of just restricting food. You’re not trying to force weight loss through willpower and calorie deprivation. You’re correcting the hormonal signals that were driving weight gain in the first place.
The Path Forward
So does insulin resistance cause weight gain? Yes, absolutely. Now you understand exactly how: by locking fat inside your cells, driving relentless hunger, and suppressing your metabolism. That’s the trap.
But here’s the way out. Lower insulin by addressing the root causes, not by simply cutting calories harder. Focus on food quality and meal timing. Build muscle. Manage stress. Give your body the conditions it needs to restore normal insulin sensitivity.
This isn’t about willpower failing you. Your body was fighting against broken signals. Fix the signals, and weight loss becomes possible again.
The scale doesn’t have to stay stuck.
Your Body Is Talking: A Pharmacist’s Guide to Stopping Prediabetes is a free guide that explains exactly what’s happening — and what to do about it. No meal plans. No shame. Just clarity.
You can also read my previous post on what insulin does to your body to understand more about how this hormone affects your metabolism and health.
Once you understand what’s actually happening in your body, you can start working with your biology instead of against it.
Medical Disclaimer
This blog post is for educational and informational purposes only and is not intended as medical advice. I am a licensed pharmacist sharing evidence-based health information, but I am not your healthcare provider.
If you have been diagnosed with insulin resistance, prediabetes, diabetes, or any other medical condition, consult with your doctor or qualified healthcare professional before making changes to your diet, exercise routine, or medication regimen. Individual health circumstances vary, and what works for one person may not be appropriate for another.
The information provided here is based on current scientific understanding and clinical evidence, but it does not replace personalized medical guidance from a healthcare provider who knows your complete medical history.
If you experience any concerning symptoms or have questions about your specific health situation, please seek professional medical advice.
References:
- Freeman, A.M., Acevedo, L.A., & Pennings, N. (2023). Insulin Resistance. In StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing. Available from: https://www.ncbi.nlm.nih.gov/books/NBK507839/
2. Sutton, E.F., Beyl, R., Early, K.S., Cefalu, W.T., Ravussin, E., & Peterson, C.M. (2018). Early Time-Restricted Feeding Improves Insulin Sensitivity, Blood Pressure, and Oxidative Stress Even Without Weight Loss in Men with Prediabetes. Cell Metabolism, 27(6), 1212-1221.e3. https://doi.org/10.1016/j.cmet.2018.04.010
