
If you’ve been hearing about fasting everywhere lately, you’re not alone. Your gym buddy swears by 16:8. Your colleague skips breakfast and says he’s never felt better. And somewhere in the back of your mind, you’re wondering: does fasting lower blood sugar levels, and more importantly, is it actually safe for someone like me?
The short answer is yes. However, fasting only works in your favour when you understand what’s actually happening inside your body. As a pharmacist with nearly two decades of experience, I’ve watched patients dive into fasting protocols without that understanding — and end up frustrated, exhausted, or worse, with blood sugar swings they didn’t expect.
So let’s sort this out properly.
Important before you continue: Fasting is a powerful tool — but it’s not suitable for everyone, particularly those on certain medications. If you take a sulfonylurea (such as glimepiride, gliclazide, glipizide or glyburide), insulin, or any blood pressure medication, please consult your doctor or pharmacist before changing your eating pattern. Fasting on these medications without guidance can cause dangerously low blood sugar (hypoglycemia). If you’re on Metformin alone, your risk is much lower — but a conversation with your pharmacist is still worthwhile.

Does Fasting Lower Blood Sugar Levels — Or Is It More Complicated?
The honest answer is both. Fasting does lower blood sugar levels for most people — but the how and why matter enormously, especially if you have prediabetes.
What Actually Happens to Blood Sugar When You Fast
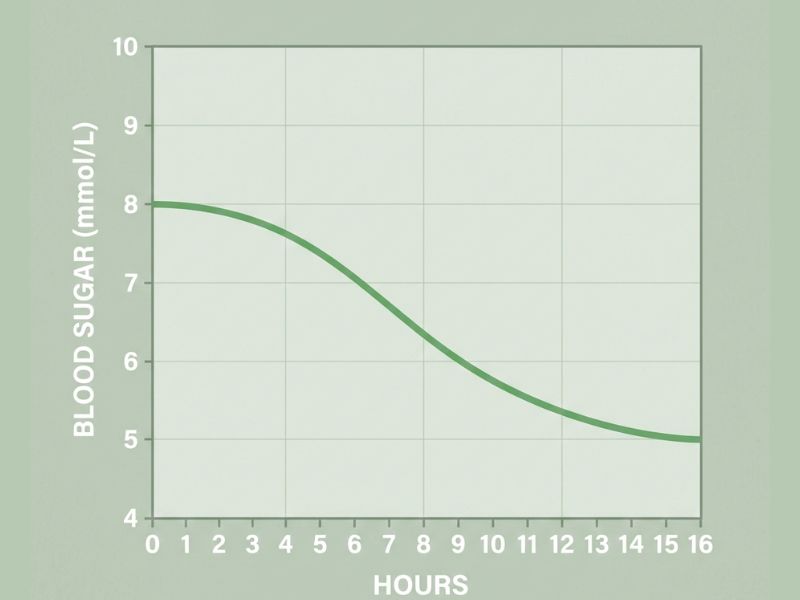
When you stop eating, insulin levels begin to drop. As this happens, your body starts drawing on the glucose already circulating in your bloodstream while your liver simultaneously begins releasing stored glycogen to keep your brain and body fuelled. It’s a smooth, overlapping process — not a strict sequence. As another pancreatic hormone called glucagon rises, it signals the liver to keep releasing that stored sugar to maintain your energy.
As your fast continues and glycogen stores deplete, blood sugar gradually settles lower. Meanwhile, because insulin stays low for an extended period, your cells get a genuine rest from constant insulin stimulation. Over time, this rest period can improve how well your cells respond to insulin — which is exactly the problem at the root of prediabetes.
Why Fasting Affects Everyone Differently
Here’s where it gets nuanced. Two people can follow the exact same fasting protocol and get completely different results. That’s because your stress levels, sleep quality, cortisol patterns, and even your meal timing history all influence how your body responds.
Furthermore, if you’re already under significant stress — long retail shifts, poor sleep, family pressure — fasting can actually raise cortisol levels, which in turn raises blood sugar. So the protocol that works brilliantly for your gym buddy may not work the same way for you. We’ll come back to this important point shortly.
The Three Most Common Fasting Protocols — and How Each Affects Blood Sugar Levels
Before choosing a fasting approach, it helps to understand what each one actually involves. So let’s break them down in plain language.

16:8 — The Most Popular Method for Lowering Blood Sugar Levels Through Fasting
The 16:8 protocol means you fast for 16 hours and eat within an 8-hour window. For example, you eat between 12pm and 8pm, then fast until noon the next day. Consequently, you skip breakfast and have your first meal at lunchtime.
This is the most widely researched fasting method for blood sugar control. Studies show it can meaningfully reduce fasting glucose levels and improve insulin sensitivity over 8–12 weeks. It’s also the most sustainable for most people because you’re essentially just extending your overnight fast by a few hours.
5:2 — Does This Approach Lower Blood Sugar Levels Over Time?
The 5:2 approach means you eat normally five days a week and restrict calories significantly — around 500–600 calories — on two non-consecutive days. So you might eat normally Monday, Tuesday, Thursday, Friday and Sunday, and restrict on Wednesday and Saturday.
Research suggests 5:2 can lower blood sugar levels over time, though results tend to be slightly less consistent than 16:8. If daily fasting feels too rigid, this approach may suit you better. That said, the two low-calorie days can increase cortisol if you’re already stressed — something to watch carefully.
12-Hour Fast — The Gentlest Way to Start Lowering Blood Sugar Levels
The 12-hour fast simply means finishing dinner by 8pm and not eating again until 8am. In other words, you stop eating after supper and have breakfast at the normal time.
This is the gentlest entry point for prediabetics. Although it sounds too simple to make a difference, research shows even a consistent 12-hour overnight fast improves metabolic markers over time. It’s also the lowest-risk option if you’re new to fasting or managing blood sugar actively.
Fasting and Insulin Resistance — The Real Connection
Understanding fasting and insulin resistance together is where the real power lies. Because fasting doesn’t just lower blood sugar — it addresses the underlying mechanism causing it to be high in the first place.
How Fasting Interrupts the Insulin Resistance Cycle in Prediabetes
Insulin resistance means your cells have stopped responding properly to insulin’s signal. As a result, your pancreas pumps out more and more insulin trying to get glucose into your cells — and eventually it can’t keep up. That’s the prediabetes trajectory.
Fasting interrupts this cycle. When you extend the time between meals, insulin levels drop and stay low for longer. Consequently, your cells get a genuine rest from constant insulin stimulation. Over weeks, this rest period helps restore insulin sensitivity — meaning your cells start responding to insulin properly again.
Why Reducing Your Eating Window Matters More Than Cutting Calories
This is one of the most important insights from recent research on fasting and insulin resistance. The timing of your eating matters as much as the content. Even without changing what you eat, simply compressing your eating window gives your metabolic system a meaningful recovery period.
Therefore, you don’t need to overhaul your entire diet on day one. Starting with a consistent eating window — even 12 hours — creates real metabolic benefit while you build the habit.
Does Fasting Lower Blood Sugar Levels Safely for Prediabetics?
This is the question you are really asking. And the answer is yes — with one important caveat.
The Morning Cortisol Problem — When Fasting Can Push Blood Sugar Levels Up

Here’s something most fasting articles don’t tell you. Your cortisol levels are naturally highest in the morning — this is called the cortisol awakening response. Cortisol raises blood sugar. So if you’re already stressed, skipping breakfast can send cortisol even higher.
Here’s why: when you wake up stressed, your body is already in a mild fight-or-flight state. Skipping breakfast can be perceived as an extension of that threat — no food available, danger must be present — which prompts your adrenal glands to release even more cortisol.
For someone with insulin resistance, this cortisol-driven glucose spike can be more pronounced and last longer, resulting in a higher fasting reading the next morning rather than a lower one.
This is why some prediabetics try 16:8 and feel worse, not better. If this happens to you, it doesn’t mean fasting doesn’t work — it means the 16:8 protocol isn’t the right fit. A 12-hour fast finishing at breakfast, or an earlier eating window, may serve you better.
Warning Signs That Fasting Isn’t Lowering Your Blood Sugar Levels as Expected
Watch for these signals that your current approach needs adjusting:
- Feeling shaky, irritable or lightheaded during the fasting window — if this happens, act immediately. Check your blood sugar if possible. If it’s low, treat it with 15g of fast-acting carbohydrates first — glucose tablets, a small glass of juice, or a few jelly sweets. Wait 15 minutes, then recheck your blood sugar. If it’s still low, treat again with another 15g. Once stable, follow up with a protein-rich snack. Protein alone won’t raise blood sugar quickly enough in a true hypoglycemic episode.
- Blood sugar readings higher in the morning than before you started fasting
- Intense sugar cravings immediately after breaking your fast
- Disrupted sleep or waking at 3am
If you’re experiencing any of these, it’s worth checking whether stress or poor sleep is interfering with your results before abandoning fasting altogether.
If this all feels a bit overwhelming, you’re not alone.
Your Body Is Talking: A Pharmacist’s Guide to Stopping Prediabetes is a free guide that explains exactly what’s happening — and what to do about it. No meal plans. No shame. Just clarity.
The FAST Method — How to Find the Right Protocol for Lowering Your Blood Sugar Levels
Rather than copying someone else’s protocol, use this simple framework to find yours.

F — Find Your Eating Window
Start by mapping your current eating pattern honestly. When is your first meal? When is your last? Most people discover they already have a natural 10–12 hour eating window. Therefore, your starting point isn’t as far away as you think.
A — Adjust for Your Stress Levels
This is the step most fasting guides skip entirely. However, your stress load directly affects which protocol is safe for you. High-stress lifestyle? Start with 12 hours. Lower stress, better sleep? You can experiment with 14–16 hours more safely.
S — Start With 12 Hours Before Going Longer
Regardless of your stress levels, start with 12 hours for at least two weeks before extending your fasting window. This gives your body time to adapt without triggering a cortisol response that works against your blood sugar goals.
T — Track Your Blood Sugar Response
The only way to know if fasting is lowering your blood sugar levels is to measure it. Check your fasting glucose first thing in the morning — before eating or drinking anything other than water. Track it for two weeks. Consequently, you’ll have real data rather than guesswork telling you whether your approach is working.
What to Eat When You Break Your Fast to Keep Blood Sugar Stable
How you break your fast is just as important as the fast itself. In fact, a poor choice at this critical moment can instantly undo the blood sugar benefits you’ve worked so hard to create.
Foods That Protect Your Blood Sugar Levels After Fasting

Break your fast with protein first. Think two scrambled eggs with a handful of spinach, a Greek yoghurt with a few berries and a small handful of nuts, or a small portion of chicken with roasted vegetables. Protein slows glucose absorption and prevents the sharp blood sugar spike that can follow a fasting period.
Furthermore, a short walk after your first meal — even 10–15 minutes — dramatically improves how your body handles the glucose from that meal. This is one of the most powerful and underused tools for prediabetics.
The Worst Things to Eat When Breaking a Fast
Avoid fruit juice, white bread, cereal or anything high in refined sugar as your first meal. After a fasting period, your body absorbs glucose rapidly — so a high-sugar first meal creates a sharper blood sugar spike than it would at any other time of day.
Similarly, a large meal immediately after a long fast overwhelms your digestive system and drives a significant insulin response. Instead, start with something moderate in size and nutrient-dense.
How Long Before Fasting Lowers Blood Sugar Levels Noticeably?
This is the question of patience — and you deserve an honest answer.
What the Research Says About Fasting and Blood Sugar Timelines
Most studies on fasting and blood sugar show meaningful improvements in fasting glucose levels between 4 and 12 weeks of consistent practice. However, some people notice changes within the first two weeks, particularly in how stable their energy feels throughout the day.
The key word is consistent. Fasting three days one week and skipping it the next produces minimal results. Therefore, a modest protocol done consistently will outperform an aggressive protocol done sporadically every time.
Why Consistency Matters More Than the Perfect Protocol

Here’s the truth about fasting that most health content won’t tell you: there is no perfect protocol. The best fasting approach is the one you can actually sustain given your work schedule, stress levels, family life, and how your body responds.
As a result, the goal isn’t to find the ideal fasting protocol immediately — it’s to find a starting point, stay consistent for four weeks, measure your blood sugar response, and adjust from there. That’s how sustainable change actually works.
The Bottom Line — Does Fasting Lower Blood Sugar Levels?
Yes — when it’s matched to your body, your stress load, and your real life.
You don’t need the perfect protocol. You need your protocol — the one that fits between your shifts at work, accounts for your stress levels, and gives your body the recovery time it needs to start responding to insulin properly again.
Start with 12 hours. Be consistent. Track your numbers. Adjust based on what your body tells you.
The framework is simpler than the internet makes it look. And if you’re managing prediabetes, you don’t need to figure it all out at once — you just need to take the next step.
Medical Disclaimer: This blog is for educational purposes only and does not constitute medical advice. If you have prediabetes, diabetes, or any other medical condition, please consult your healthcare provider before beginning any fasting protocol.
References
Sutton, E.F., Beyl, R., Early, K.S., Cefalu, W.T., Ravussin, E., & Peterson, C.M. (2018). Early time-restricted feeding improves insulin sensitivity, blood pressure, and oxidative stress even without weight loss in men with prediabetes. Cell Metabolism, 27(6), 1212–1221. https://pubmed.ncbi.nlm.nih.gov/29754952/
Wilkinson, M.J., Manoogian, E.N.C., Zadourian, A., Lo, H., Fakhouri, S., Shoghi, A., Wang, X., Fleischer, J.G., Navlakha, S., Panda, S., & Taub, P.R. (2020). Ten-hour time-restricted eating reduces weight, blood pressure, and atherogenic lipids in patients with metabolic syndrome. Cell Metabolism, 31(1), 92–104. https://pubmed.ncbi.nlm.nih.gov/31813824/
